In my speeches about transforming healthcare I sometimes speak about mashups: combining several things that were created without knowledge of each other, creating something new. One example is satellite navigation systems in our cars: when those GPS (global positioning) satellites were shot up in the air, nobody had the idea of combining their data with street maps and combining that with way-finding software, to help us get from wherever-we-are to wherever-we-want-to-be. Mashups are one of the key methods of improving the value of things, especially on the internet.
In my talks I say that I can't wait to see what mashups will do for healthcare - but it all depends on the ability to move data between systems, so smart innovators can add value to it. If the data's in silos, mashups can't happen.
Well, there are other kinds of mashups. Here's one, courtesy of fellow kidney cancer patient and ACOR member Richard Catlett, via his Facebook page: Laurel and Hardy meet Santana - clearly two performances that were never destined to meet. Except on the internet. (Email subscribers, if you can't see the video, click here to come online and view it.)
p.s. This is my personal blog about healthcare issues. My business website and blog is ePatientDave.com.
Friday, November 19, 2010
Laurel & Hardy meet Santana: a mashup
-
e-Patient Dave
-
6:10 PM
![]() 1 comment
on this post (Click to view or add one)
1 comment
on this post (Click to view or add one)
Tuesday, October 5, 2010
US Military Pursues Patient Engagement
I had an amazing experience last Thursday. I encountered some of the smartest, fastest-thinking, most motivated healthcare transformation thinkers I've ever seen. The ideas were flying so fast it was like transformation popcorn. And this was in an organization I'd never heard discussed as health leaders: a U.S. Army "Physician Champions" meeting in Boston.
The people I met with have a particularly passionate commitment to effective care: having chosen the military themselves (not the world's best working conditions), they're distinctively committed to their patients. They have a long-running EMR system (electronic medical record), so that any "doc" who encounters a patient can see what previous providers have entered. And because of frontline military circumstances (at the front, a medic is the one you call "doc"), the records are used by all tiers of providers. In these conditions the value of accurate information is acutely apparent - as are the challenges of system usability and workflow.
The event leaders who invited me to speak were as passionate about patient engagement as anyone I've met anywhere. I spoke about participatory medicine, and heard discussions of real-world workflow issues and best practices for working with the system to get the job done. It was concrete and practical.
I had a strong sense that U.S. hospitals will have lots of meetings like this in the next few years as they implement EMRs.
I wondered why in all our civilian discussions of EMR I haven't heard of this group of change leaders. Sure, I've heard about the DOD's long-standing use of their medical record, and I know about the VA's system (which is not the same as DOD's). But I had no idea there was a group aggressively advocating for patient engagement in the military.
And to me that makes a ton of sense, because for the most part, when soldiers leave the service their medical record will no longer be visible to their new providers. They'll need to be engaged in their care.
My gratitude to Dr Bob Walker from the Europe Army Medical Command in Heidelberg and his team for introducing me to this special operation. Great people with an inspiring passion.
-
e-Patient Dave
-
10:39 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
Monday, October 4, 2010
Vigil for Tyler Clementi and gay teen suicides
Last month Rutgers freshman Tyler Clementi was secretly observed, via webcam, in a sexual encounter with another man. The encounter was streamed over the internet and tweeted by his college roommate. On September 22 Tyler killed himself. (Wikipedia)
Readers of my book know that a powerful force in my cancer story was my sister Suede (website), a jazz and blues singer based in the Provincetown, Massachusetts area with a profound respect for human. Last Friday she participated in an impromptu vigil for Tyler and the four other gay teens in the U.S. who reportedly killed themselves in September.
Here's an informal video of the vigil. Suede is briefly seen in the beginning, as she sings John Calvi's "The Ones Who Aren't Here," from her first album. The song was written about and recorded during the worst of the AIDS epidemic. The quality's not great - Suede was standing on a park bench, playing through a battery powered amp - but the message is authentic. The speaker is Suede's friend Bradley, who organized the gathering.
(Email subscribers, if you can't see the video, click here.)
I ask that we honor humanity in all its diversity and variation, and that we teach our youngsters, even rambunctious teens, to do the same. This is no joke.
-
e-Patient Dave
-
9:32 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
Saturday, September 11, 2010
MITSS seeks HOPE Award Nominations
Do you know someone, patient or professional, who's been involved with medical error and has responded to it in a powerful, productive way? Please nominate them for this award.
MITSS is a tiny, wonderful, much-needed organization that does good work in an important area we hardly ever hear about: they provide services for people traumatized by medical error. And that includes both the patient/family part of it, and the clinicians who made the mistake. I first wrote about them last fall on e-patients.net, then attended their annual fundraising dinner. At this year's dinner, November 4, I have the honor of delivering the opening remarks.
Nominees are open, through 9/15, for their annual HOPE award. I lifted this from Paul Levy's blog: MITSS HOPE Award Nomination Deadline -- September 15, 2010
MITSS HOPE Award Nomination Deadline -- September 15, 2010
The deadline for sending in your nomination for the 2010 MITSS HOPE Award is fast approaching. Take the time to nominate an individual, organization, department, or group that is doing great work aligned with the MITSS mission of Supporting Healing and Restoring Hope to patients, families, and clinicians impacted by adverse medical events.
Along with the national and international recognition that this prestigious award affords, the winner will receive a $5,000 cash prize that has been provided by the award sponsor, rL Solutions.
Go here for award criteria, an online nomination form, award history, past winners, and more! Nominating someone is easy, and submissions are done entirely online. Remember, too, that self-nominations are acceptable. Contact Winnie Tobin at (617) 232-0090 if you have any questions.
ABOUT MITSS: Medically Induced Trauma Support Services (MITSS), Inc. is a non-profit 501(c)(3) organization headquartered in Chestnut Hill, MA, whose mission is "To Support Healing and Restore Hope" to patients, families, and clinicians whose lives have impacted by medical errors and adverse medical events.
-
e-Patient Dave
-
8:19 AM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Monday, August 30, 2010
My review of Elizabeth Cohen's book "The Empowered Patient"
 This month CNN Senior Medical Correspondent Elizabeth Cohen released her first book, The Empowered Patient: How to Get the Right Diagnosis, Buy the Cheapest Drugs, Beat Your Insurance Company, and Get the Best Medical Care Every Time. I got an advance review copy, and it's taken me this long to figure out how to express my thoughts. I just posted this review on Amazon.
This month CNN Senior Medical Correspondent Elizabeth Cohen released her first book, The Empowered Patient: How to Get the Right Diagnosis, Buy the Cheapest Drugs, Beat Your Insurance Company, and Get the Best Medical Care Every Time. I got an advance review copy, and it's taken me this long to figure out how to express my thoughts. I just posted this review on Amazon.
_______
I've always been an empowered patient, so I didn't need to be sold on the concept. I'm a cancer-beating patient blogger, I'm co-chair of a medical society about doctor-patient partnerships, and I wrote my own book. So my question was, what does this book bring that's new?
What it brings is convincing stories, clear explanations, and concrete how-to's. It's short, comprehensive, and convincing. I don't see how you can NOT read it if you're responsible for someone's care, including your own. It awakens you to possibilities and risks, leaving you aware and enabled.
(Disclosure: Cohen wrote a quote for the jacket of my book, which is selling a million times slower than hers. But her view is different from mine. I've worked for weeks figuring out how to express the differences here.)
I'll start with the author's challenge, then how she handles it, then my objections.
The first big challenge for an author in this space is that *people tend not to care* about quality until trouble hits. And when it does, there's an instinct to not rock the boat: people want to stay put, to believe they're getting the best care possible. It's not rational, but I've seen it repeatedly: people are loathe to step out of the boat they're in, especially in troubled waters.
It's hard to hear that care might fall short, but it can. And there are many causes: human fraillties, lagging technology, information overload, even business ethics.
And here's the author's dilemma: the better you prove this with story after story, the more readers might feel powerless and turn away.
So how do you reach people?
This is where Cohen's mass media skills come in. She knows how to tell a story concisely, dip into the underlying reasons, and come back up with some concrete "Here's what to do's." There's an art to this: her own stories about her baby and her mother sometimes brought me to tears, but I wasn't turned away as I sometimes am. I was left feeling *this stuff matters*, and patients can help. By wising up, thinking for themselves, and speaking up.
Objections: if Amazon had a 100-point scale I'd give it a 95, not 100. First, a stylistic nit: it's obviously written by a TV person. Time after time she injects, "Coming up, I'll tell you how you can xyz"; I could almost hear "...right after this message." But people who think "She can't be serious, she's on TV" are wrong: every one of her anecdotes rings true, based on the many people I've met at conferences, and almost all her "What you can do's" are spot-on.
I agree with Mack90's comment that dot-gov sites are not quite as valuable or perfect as the book suggests: they can lag behind or be editorially skewed, no guarantee of "bestness." I've seen plenty of outdated information about my own disease (kidney cancer) on sites that match her recommendations, including sites with seals such as HON. But I don't feel as strongly about this as Mack90 does.
Finally, I object pretty strenuously to the title of the opening chapter: "How to be a `bad' patient." I'm clear that Cohen's intent (as she said yesterday in the New York Times) was to reach people where they are - speaking into the mindset of the mass market she talks to professionally, where many people feel it's not good (or even safe) to question one's doctor. I get the point, but I would have preferred to word it "It's *OK* to be a `bad' patient." In my view, "how to be bad" is a rough start for a book about empowerment.
But that brings me back to the top: this book brings mass-market communication skills to an area where many of us have worked hard to wake people up. Our books have contained much more information from different angles, but this could be the breakthrough that opens millions of minds.
-
e-Patient Dave
-
7:00 AM
![]() 1 comment
on this post (Click to view or add one)
1 comment
on this post (Click to view or add one)
Sunday, August 29, 2010
An interlude for laughter, the best medicine
I used laughter when facing my cancer, then put it in the title of my book.
This is from Uncle Sandy in Atlanta. Get ready.
(Email subscribers, if you can't see the video, click the headline to view it online.)
-
e-Patient Dave
-
11:24 AM
![]() 3 comments
on this post (Click to view or add one)
3 comments
on this post (Click to view or add one)
Saturday, August 28, 2010
"Compliance: It's Not Just for Patients Anymore."
I'm in a patient safety workshop in Boston today, about engaging minorities in safer care. We just saw a video about safety awareness, encouraging patients to realize what a good role they can play in helping clinicians (doctors and nurses) get everything right. (Long story short, there are many many ways that things can and do go wrong - some complicated, some simple.)
When people talk about making healthcare more effective, "compliance" often comes up. It's usually about whether you and I take our pills, improve our diet, etc. Patient compliance is a hot topic on blogs: Google shows 93,000 blog posts, and 9,000 in the past year.
But the video made a thought come up: holy cow, a lot of healthcare quality issues are because clinicians forget to fulfill their part of the plan. Ironic! But fault-finding finger-pointing doesn't produce behavior change as well as inspiration does - calling forth what people know to be the best in themselves. Here's a draft of a message we might want to spread - feel free to share:
"Compliance: It's Not Just for Patients Anymore."
We all know about patient compliance: whether patients follow our instructions to accomplish good care. When compliance falls short, our profession is undermined. Care suffers, and our efforts are frustrated.
The same is true when we don't comply with our part. Whether it's hand washing or the Five Rights of administering medications, any shortfall cheats the profession as well as the patient. And perhaps our diligence - or lack of it - even rubs off on patients.
Compliance isn't just for patients anymore. Let's not cut corners. Let's set a great example for every patient, and stick to the plan.
This text authored by "e-Patient Dave" deBronkart. May be posted & shared freely with this attribution intact (Creative Commons Share-Alike 3.0)
Additional resources:
- The safety awareness video is in this e-patients.net post.
- MITSS, the sponsor of this workshop, is here.
- The "five rights of medication administration" are:
- The right patient (this is why they constantly ask your name and date of birth)
- The right drug (medications too often get mixed up)
- The right dose (Dennis Quaid's newborn twins famously almost died because two bottles of medication looked too similar though one was 1,000 times stronger)
- The right time (4x/day, before meals, etc)
- The right route (pill vs IV, etc)
-
e-Patient Dave
-
12:03 PM
![]() 7 comments
on this post (Click to view or add one)
7 comments
on this post (Click to view or add one)
Friday, August 13, 2010
Are you happy about why you're here? Are you free to be?
TED talk by Elizabeth Gilbert. Love this quote:
"Is it rational, is it logical, that anybody should be expected to be afraid of the work that they feel they were put on this earth to do?"
I'm posting it because the work I'm doing now is so fabulous, such a self-expression, that I get what she means. As it says on my business website, “This is the first time in my life I’ve felt I have a calling,” says Dave, “something I can’t get away from: it’s what I need to do. I’ve had plenty of fulfilling jobs in a great career, but not a calling. This is it.” And I think everyone should be on the lookout for what calls to them - like the muse she describes that flew into Tom Waits's head while he was driving, or the one that pulled the poet home to grab a pencil and pull that verse out of the air. Backwards, if necessary, as it tried to get away.
I know the feeling described in this talk, of a message coming through me, in a way that I just grab as it goes past. And when I speak, I just say what apparently is waiting to be said.
I'm going to watch this over and over. Thanks for the support you all give me, and special thanks to high school classmate Susan Alnes for steering me to this.
-
e-Patient Dave
-
12:03 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
Wednesday, August 4, 2010
What's new in the new life of e-Patient Dave
- The big news is that my book was released a month ago: Laugh, Sing, and Eat Like a Pig: How an empowered patient beat Stage IV cancer (and what healthcare can learn from it).
- Here's the listing on Amazon, and reader reviews. (Conference producers, visit my contact page to ask about bulk purchases.)
- Here's the listing on Amazon UK.
- Here's the book's website. (At present it's a subset of my larger website; soon it will have its own.)
- The advance praise has been inspiring.
- I've traveled a lot in recent months, speaking, attending policy meetings in DC, and meeting with people doing good work in healthcare. My schedule page is here.
- One of my favorites is that in October I'll be attending the fabulous TEDMED conference in San Diego, serving as an analyst for the Robert Wood Johnson Foundation. These are truly wonderful people with [big] fingers in many great healthcare projects, including Aligning Forces for Quality - a multiyear project that's already developing great data on how we can do healthcare better.
I'm particularly grateful to Klick Pharma, my client who produced the superb short version of my long story, which I posted here in June. They're exquisitely skilled, they really get it about patient engagement, and they're carrying the message forward skillfully.
Thanks to all of you who've been so supportive and encouraging - especially you who've provided paying work, to keep this "project" alive. Here's to better health for all!
-
e-Patient Dave
-
9:11 PM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Wednesday, July 21, 2010
Boston Globe notices my fabulous singer sister Suede! Cape Cod Jazz Festival, tonight
 Long-time readers of this blog - and readers of my book(!) - know that a powerful force in my disease process was my Cape Cod jazz/blues singer, Suede. A totally self-supporting independent musician for years, today she finally burst onto the pages of "g," the Boston Globe's daily magazine of entertainment and diversion.
Long-time readers of this blog - and readers of my book(!) - know that a powerful force in my disease process was my Cape Cod jazz/blues singer, Suede. A totally self-supporting independent musician for years, today she finally burst onto the pages of "g," the Boston Globe's daily magazine of entertainment and diversion.
Writer June Wulff seems to have newly discovered my baby sister, but she totally gets it: "Watch out ... oy, we're in love with this talented lady." Couldn't have said it better myself!
One night only, at the Cape Cod Jazz Festival in Chatham, MA.
And it's FREE! (Usually a Suede ticket is $20-60.) FREE!
-
e-Patient Dave
-
9:34 AM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Wednesday, July 7, 2010
Kids are invited to say what THEY want from next-generation healthcare (free webcast)
I know this is last-minute but we/they don't have many registrations. If you know a kid, age 5 to anything, who's free Thursday afternoon July 8, join this free webcast. It's from 2:00-5:00 Eastern, and it's fine to attend for part of the event.
The webcast series: "Person Centered Health."
This is a great group of people, mostly in Canada, whom I met through my primary physician, Dr. Danny Sands. Why "person centered" instead of patient centered? Because they're way outside the box where most of us live; to them healthcare is not just part of good health, it's part of a good life. (I gave a brief glimpse of it last month, after speaking at a Toronto meeting.)
They run a monthly webinar that's unlike anything I've seen. It's a free live Webex event, which you can join by phone like a usual Webex. Or, if you're near a Cisco office (they own Webex), you can participate using their incredible "Telepresence" room, with life-size monitors. I participated in one of these, and it really is like being in a room with the people in other cities. It's nothing like Skype video.
In either case, you can register here. Now for the good stuff:
This session:
At the last session, even these out-there thinkers felt cramped, and wondered: What if we got some kids in here and asked them what they think? So at tomorrow's session, kids are invited to speak up. (I apologize for the late notice but I just realized yesterday that there's been little promotion and only two kids have registered so far.)
Organizer Wayne Mills writes this description:
As you know, Person Centered Health is a journey. In the past few months we’ve had some excellent speakers give us their perspective in how to enable PCH from a policy stand point, from an operation stand point, from a patient standpoint. One critical group we have yet to hear from is the people whom will have to ensure Person Centered Health is delivered in the future.
Therefore for our next session scheduled for July 8th at 2 PM Eastern time, we would like to invite young people. We would like to learn how do they see participating in their own healthcare system? Are they going to participate in the same format as we are (i.e. agree to have a wait time in their healthcare system) or are they going to create their own systems via social networking, etc? What changes would tomorrow’s leader's demand from today’s system?
Again, register here. It's even okay to register and join after the session starts. What's important is participation.
-
e-Patient Dave
-
5:31 PM
![]() 1 comment
on this post (Click to view or add one)
1 comment
on this post (Click to view or add one)
Tuesday, July 6, 2010
I used to hate Thunderbird. Is it better now?
This post is for people who've used the Mozilla Thunderbird email program, and are fairly demanding. Because I'm a demanding email user, and I'm considering Thunderbird.
But when I've tried it I've hated it, and I wonder if it's improved. A lot.
Background:
The other day I asked for help on improving my email situation. I got great advice, and I'll be moving to Google Apps, as several suggested. Tom Iglehart, co-chair of CCTWG, will help me with the move.
Here's the geek part: I currently use Outlook Express, but Tom points out that if I move to an app that supports IMAP, I'll be able to view all my emails (received and sent) from any device or any computer. (Why do I care? Among other things that will let my wife comb through email conversations about speaking engagements etc, which will take a big burden off my sole-proprietor plate. She's infinitely better than me at detail work.)
The best known app that supports IMAP is Outlook. I hate it. In my experience (three times over the years) it gets full and then it starts malfunctioning, and I'm not interested in putting in the effort to become expert at managing a dysfunctional program.
Several times I've tried using Mozilla Thunderbird instead. It was funky but okay, but there were infuriating limitations (really dumb missing features), which caused me every time to punt it and go back to Outlook, because my employer required it. Now that restriction's gone.
So I need to know, is Thunderbird a lot better than it used to be?
-
e-Patient Dave
-
2:07 PM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Labels: infrastructure
Friday, July 2, 2010
"Think About Your Life" patient-driven website
I love this: a website that could ONLY have been created by cancer patients.
http://www.thinkaboutyourlife.org/
"Find empowerment: Anything you can do to feel like you are taking control of your illness and treatment will help you. Thinkaboutyourlife was developed by cancer survivors. We have used the tools on this website in our own experiences, and we hope to inspire you do the same.I learned about the site from its creator, Amanda George, who commented on last month's post about person centered health. Hot diggety. Doncha just love how the internet is letting us connect with each other and share ideas??
This website provides easy to use tools for each stage of the cancer journey to help you:
- Process your thoughts and feelings:
Elizabeth shared the "Good day, bad day" tool with her family to tell them how they could help her throughout treatment.- Take control and make decisions:
Amanda used her "One Page Profile" with her doctor to discuss the impact of treatment on her life.- Think about the "what now" and the "what next"
The "Hopes & Fears" tool helped Susan to think about the next few months of her life after treatment.
-
e-Patient Dave
-
4:08 PM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
I need a new email hosting company. Suggestions?
This one's for people who know about how to host websites etc. I need a change.
For www.ePatientDave.com I'm using an inexpensive hosting company, GoDaddy, that has great customer service. I'm not thrilled by their using Danica Patrick as their spokesperson in a cheesy way, but I can tolerate it. They've got really good customer service: competent people on the phone with little or no hold time. Their technical web interface is a mess in my view, but they're willing to do everything for you over the phone.
I've registered my domain name with them, and my website lives on their computers. Other users have mentioned that their sites have gone down occasionally but it's working fine for me.
What's not working fine is the other service I buy from them: email hosting. The way they do it, my genuine emails look like spam or phishing to some filters - and that keeps me from reaching clients. Like, when I try to email anyone at the Mayo Clinic it gets rejected.
Another client, potentially my biggest ever, thought I had no interest. They called before giving up, and we discovered all 5 of my responses had gone into their spam folder for the same reason.
Here's the corker: when I called in to ask Godaddy about it, the well-meaning guy on the phone was naive enough to say, "Well, your email is legitimate - can't you tell the Mayo Clinic to change their security settings?"
Right. Uh-huh. No, I think it's time to get rid of you, Godaddy, and find a provider who understands email security issues.
Suggestions, anyone?
I'm willing to consider Gmail, but I don't know if it's industrial strength. Ideally I'd like a provider that lets me store virtually unlimited emails on the Web, so my staff can access them - but it's vital that I have a copy on my computer too, so I can read them offline.
-
e-Patient Dave
-
3:11 PM
![]() 9 comments
on this post (Click to view or add one)
9 comments
on this post (Click to view or add one)
Labels: infrastructure
Saturday, June 26, 2010
Coverage of ePatient conference at the National Library of Medicine
This spring I had the thrill and honor of being invited to speak at the National Library of Medicine in Bethesda, Maryland. Why? Because they actually had a conference about e-patients.
Yes, the U.S. National Library of Medicine, part of the National Institutes of Health, had an e-patient conference.
And they brought all the brass. Here's the inside front cover of the current issue of Medline Plus, their (free) magazine: (click to enlarge)
This was one of several times I found myself crossing paths recently with David Blumenthal. Funny, when he was a doctor at Mass. General I never saw him, but now I see him often.
The most fun was meeting Dr. Lindberg, quoted in the article. In every speech I cite something he said that's quoted in the e-Patient White Paper, about how impossible it is for doctors to keep up with the information explosion:
"If I read two journal articles every night, at the end of a year I'd be 400 years behind."That's one of the most potent quotes to open people's minds to the power of activated, engaged, e-patients. Physicians are overloaded and have thousands of conditions to track; you and I only have our own conditions. They must go wide; we can go deep.
The really fun thing is this: sometimes a skeptic would question Dr. Lindberg's statistic, saying "That's not really true - it's probably different today." Well, now I can say "When I had dinner with Dr. Lindberg this spring, I asked him about that. He said it is different: it's much worse now."
Here's to e-patients - and here's to the amazing realization that these great academics are noticing!
-
e-Patient Dave
-
10:28 PM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
It's my Drop Dead Date plus three years. Thppppt!
Three years ago today was "razzberry day," aka Drop Dead Date. So, today on my CaringBridge journal I posted this picture.
Huh?? Patience, my lovelies; all shall be revealed:
At diagnosis on January 11, 2007 my median survival was 5.5 months, which predicted an "expiration date" of June 26. On that date all my buddies gathered at noon eastern time and blew razzberries (Bronx cheers) at Death as we zoomed past it and into the future.
Here's an email Mom sent yesterday to my siblings:
"Hi, all - Saturday, June 26 is the 3rd anniversary of Dave's beating his "Drop Dead Date" of the average 5.5 months survival time after diagnosis of his particular brand of cancer. I personally plan to give the razzberry salute at noon, again, to commemorate the day, and invite you to join me...Dat's my mom - and you're my razzbuddies. Life is crazy good!
"He's at a conference in SC, home Sunday night; his book Laugh, Sing, and Eat Like a Pig is coming to Amazon SOON. I've spent the past few days doing a bit of proofing for him, and reliving the story; some tears, some giggles, lots of strong reminders of how and where we all were 3 years ago, dealing with HIS cancer, each in our own way. And the book also has much of where he's been since then... I'll (personally) make sure you each get a copy when it's published. My treat, though Dave may have had that thought already. If so, I win because I'm the mother and I said so..."
-
e-Patient Dave
-
12:56 PM
![]() 4 comments
on this post (Click to view or add one)
4 comments
on this post (Click to view or add one)
Labels: caringbridge
Thursday, June 17, 2010
A vision of *people-centered* health
Heads-up, people - this is somethin' good.
I was invited to speak today at a meeting on "Patient-Centered Health" sponsored by the Ontario Hospital Association. I was followed to the stage by Vaughan Glover, author of Journey to Wellness, a 2005 book with a terrific vision of healthcare in which patients are truly responsible for the state of healthcare.
I hope to write more about it later, but for now just savor this quote from the back cover:
"We, the patients, must lead the way in building the next generation of health care in our country. The change will be driven by an informed and empowered public, demanding access to what is possible rather than what a government or any other support group is willing or able to provide."
How could I not have met this guy before?? Glad I did.
-
e-Patient Dave
-
11:12 PM
![]() 1 comment
on this post (Click to view or add one)
1 comment
on this post (Click to view or add one)
Thursday, June 10, 2010
When BP spills coffee
From the Upright Citizens Brigade comedy site, UCBComedy.com:
(Thanks to Paul Levy for tweeting this.)
-
e-Patient Dave
-
7:49 AM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Sunday, June 6, 2010
Seven minutes of an engaged patient's story
One of my clients is Klick Pharma, a Toronto marketing firm that creates superb websites to help patients be engaged in their care. They're real professionals in all the domains of their work: human interaction (how people use a website), messaging (the way concepts are delivered in words), and every aspect of production.
This spring they invited me to their video studio to record an informal chat version of my story, highlighting the ways patients use the internet to alter how they deal with disease. We spent several hours, and they did a terrific job of editing it down into something coherent.
(Email subscribes - if you can't see the video, click the headline to view the post online.)
The same video is on Klick's site here. Also on that site is a video of a talk I gave with Klick's Brian O'Donnell at a conference in Philadelphia. Most people in pharma marketing talk about the medication itself (in one way or another); Klick's approach is to support the patient in much broader ways - "Beyond the Pill," which is the title of the talk.
My segment starts at about 9 minutes. Thanks to Klick for their patient-centered approach, their competence, and for being a client of mine (in that order).
-
e-Patient Dave
-
9:50 AM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Wednesday, May 26, 2010
Urgent call for help - rare pediatric side effect of dialysis
My social media friend Dale Ann Micalizzi sends an urgent call for help. A 3 year old's life seems to be in imminent danger
I need help for a family that I'm working with from a pediatric nephrologist specializing in dialysis where child is having a rare side effect that no one seems to have heard of before. Please email me if you know of someone willing to talk w/family or PICU or answer a few questions for me.
...
Because of this flesh eating infection, he lost all kidney function and is on dialysis. The entire doc team never heard of the reaction that he's having to the dialysis. His face turns red, he screams the entire 2 hours even though he's on high power narcotics. His heart rate races to almost 200 and becomes tachycardic and his BP drops. If you could ask your nephrology friends if they have ever heard of such a thing and what they could do to relieve his pain or if anyone would be willing to talk with the Mom so that she could feel that she tried everything to save him?
More information is in this newspaper story. (Caution - some specifics are unbearable to read, and the important info is above.)
Because time is short and I'm overseas (not online constantly) please email Dale directly: micalizzidag at AOL. Or if you know of a specialist with info, they can contact the hospital directly - the main number is 518-262-3125. The family's name is in the newspaper story.
-
e-Patient Dave
-
5:53 AM
![]() 1 comment
on this post (Click to view or add one)
1 comment
on this post (Click to view or add one)
Thursday, May 20, 2010
Leonard Cohen's "Hallelujah" as sung by my sister
When I was in college in Boston, Canadian singer-songwriter Leonard Cohen was a big deal. His dark, pensive voice and poetic lyrics set him apart from much of Sixties music.
His best-known song then was "Suzanne," but Wikipedia says in recent years it's been surpassed by his 1984 "Hallelujah." I'd never heard it until, at my sister Suede's recent concert at Boston's Sculler's Jazz Club, she pulled it out (total surprise to me) and rendered a beautiful, spiritual six minute version of it.
Suede is much loved on Cape Cod, and she sang it at an annual spring bonfire, another much-loved occasion. Perfect.
-
e-Patient Dave
-
7:10 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
Labels: Suede
Monday, May 17, 2010
CaringBridge testimonial video
Last week I wrote about my visit to CaringBridge headquarters. The night before I had an idea - why not pull out a camcorder and record an impromptu testimonial? I've been doing some video interviews lately, and they come out okay; why not give a big thank-you to the website that meant so much to me, and to my community, during my illness?
I was tired (not enough sleep that intense week!), so I was a little hoarse, but here it is. Heartfelt.
(Email subscribers, if you can't see the video, click here to view it online.)
I encourage you to send a donation to CaringBridge, small, large, or tiny. It's a darn good service, and they offer it free to anyone. And at a time of crisis, that's a big deal. You can help make it possible for more people.
-
e-Patient Dave
-
11:10 PM
![]() 1 comment
on this post (Click to view or add one)
1 comment
on this post (Click to view or add one)
Labels: caringbridge
Friday, May 14, 2010
"The poster child for patient empowerment" - Mpls Star Tribune
Well THIS is fun.
Last week I gave the keynote address at the 13th annual ICSI / IHI Colloquium - an audience of 500+ physicians, hospital administrators, health plan (insurance) executives, all focused on doing healthcare better. ICSI is forward-thinking and Minnesota-based (not surprisingly - MN is a long-time leader of better health practices), and is finally starting to get recognition outside the state. Attendance in the past has always been around 300, so it's good to see it growing.In the audience was Maura Lerner, a health reporter for the Star Tribune. We talked afterward, and she wrote a long, great piece that was on the front page of today's paper. A few details of my story are a little off, but she completely got the message right regarding patients being engaged in their health, as effective partners of their physicians.
They wanted a photo, so they came with me the next day when I visited the headquarters of CaringBridge, the wonderful website I used to communicate with family and friends during my illness. This photo is from the tour I was given by Sami Pelton, their director of partnerships. (That's her.)
______
Update 5/17: During the visit I recorded an off-the-cuff testimonial video for them. It's in my next post.
-
e-Patient Dave
-
9:55 AM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Labels: caringbridge
Friday, April 16, 2010
Book launch and jazz show April 22, Boston!
I have exciting news and an invitation to all of Boston: Please rearrange your life and join me, Thursday night at Scullers Jazz Club! The news: I’m announcing my first book. It'll be out in June. Cover art is at left.
The news: I’m announcing my first book. It'll be out in June. Cover art is at left.
It's my story then and now: excerpts from my online CaringBridge journal, interwoven with what I’ve since learned about e-patients and participatory medicine.
The title reflects the mind-powered approach I took to my “prognosis is grim” disease. (More on this below.)
The invitation is for all of New England to come celebrate and honor a singer who was a huge, powerful force during the course of the disease: my sister Suede. (Yes, that’s her name.) She’s performing Thursday, April 22 at Sculler’s Jazz Club in Boston. One show only. Tickets: http://www.scullersjazz.com/attractions/detail.htm?id=839
She’s performing Thursday, April 22 at Sculler’s Jazz Club in Boston. One show only. Tickets: http://www.scullersjazz.com/attractions/detail.htm?id=839
With four CDs and a live DVD to her credit, Suede is a self-made independent artist with a phenomenal stage presence. Be prepared to be owned by the diva for the entire evening. You’ll see what I mean.
All New England, please come join us! It’s a dual celebration – Suede rarely plays Boston (she’s more often found on Olivia Cruises), and I’ve never published a book. April 22, 8 pm. Best seats go to those who buy the dinner/show package.
Q & A follows. "Do it!," as Suede says during one of her songs. :-)
What’s the title about??
It's the approach I chose to take to the news that I had a lethal cancer - a summary of the advice I got in the first few weeks after diagnosis, before I even started my journal:
- "Laugh" is for the healing power of laughter, as famously discussed by Saturday Review editor Norman Cousins in his book Anatomy of an Illness
- "Sing" is the advice my doctor gave. I had asked if I should drop out of my much-loved championship chorus to save energy, but he said, "You don't want to stop doing life activities that you love - it sends the wrong message." Wow. So, okay, laugh and sing! Not bad.
- "Eat like a pig" refers to the diet the hospital sent me, to increase my caloric intake, to combat weight loss and prepare for the battle ahead.
Why a book with this message?
4,000 people a day (in the US alone) discover they have cancer, and face that moment of "What on earth do I do NOW??" I know that feeling. Some look for what to do next; others don't even think they can do anything — they just think they're screwed and go into depression. This book is about hope, getting it in gear, and going "e." (E-patients are "empowered, engaged, equipped, enabled, and educated.")
What does Suede have to do with it?
"Laugh Sing" is about facing the unfaceable with power and grace, and nobody was a stronger influence than my sister Suede.
She taught me to have a powerful relationship to the disease (all explained in the book) and not be owned by it. She taught me what she learned about facing death from her years working with patients in the AIDS epidemic. She brought people from her extraordinary fan base to join our support group on CaringBridge.
Most incredibly, she organized an impossible effort to solve another challenge I’ve rarely discussed: The whole time I was sick we owned an extra house.
We’d lived in the Midwest for a while before something told us we had to get home to New England. We put that house up for sale in 2006, just as the market hit the skids, though nobody knew it yet; we thought it would sell soon.
Then I found out I wasn’t getting the job that was 99% (not 100%) certain. So for months I owned two houses with no income. I found a job. And three months later I learned I had Stage IV cancer.
The value of both houses started dropping. 30%, eventually. So, while I was sick we also had carrying costs for two houses on a one-house budget. And not even any showings on the old house. It felt crushing, but we were focused on just staying alive. First things first.
Then, we got an offer. For $18,000 less than we owed.
What did Suede do? She organized an incredible campaign and put on a benefit concert – she and her community raised the $18,000. So, in September 2007 we sold that house and got the official word that I’d survived. It was a very good month.
Join us. Celebrate the book, Suede, and life!
You can see what a powerful, wonderful, amazing woman this soulful singer is. She will own you for that evening.
At the benefit concert my physician Dr. Danny Sands and wife Libby came to the first half of the show. He was blown away: at halftime they were trying to decide which CDs to buy, and they decided they had to stay for the second half to hear more songs.
That's how good she is. (He later said “We came for you, but we stayed for Suede.”)
Let’s sell out the house! Bring friends! Rearrange your life for this rare show - buy tickets. Celebrate life!
-
e-Patient Dave
-
8:36 AM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
Sunday, April 11, 2010
When I Leave the World Behind
Work is underway on a book I promised several years ago to write. It’s extracts from my cancer journal on CaringBridge - the cancer story itself, and how I used everything at my disposal to help my cause: the internet, great medical care, and the power of attitude. Woven throughout are observations on how e-patient principles are changing the process of disease (and health). At the time I’d never heard of an “e-patient,” but what my support community and I were doing exemplified it.
The book's work is being driven by my long-time associate George Alexander, who is also the publisher.
It’s been emotionally hard to dig back through those journal posts, because those were scary times. The chapter I’m working on now is about hope, so yesterday I read Jerome Groopman’s book The Anatomy of Hope. It's filled with stories of being with patients as they faced probable death, and the physician’s journey of learning to help them deal with it.
I cried as I recalled facing my own death. It was accentuated by recent events:
- Fellow kidney cancer patient Rick Schleider died last month.
- My classmate Don Levinstone lost his fight with pervasive lung cancer last month.
- Last week my dear singer-sister Suede's longtime companion dog Angel died. Angel was a miracle dog, an abused stray who lived on a highway median for months before being rescued. Suede adopted her and gave her a life she never would have known. The loss is hard on her.
- Today’s CBS Sunday Morning had a Katie Couric segment on children who lose a parent. (5% do, before age 15.) The family photos and the footage of the children’s words, their loss, brought me back to the thought of leaving my family behind.
That night I attended the annual concert of my sister Amy’s excellent Sweet Adelines chorus The Pride of Baltimore. The headline act was Wheelhouse, a champion quartet whose signature song is When I Leave the World Behind. Irving Berlin's beautiful lyrics [below] flooded me; I sat there with tears running down my face, thinking of my dad's departure from this world.
Today that song came back to me as I heard the children talk. I found Wheelhouse's performance on YouTube, and found myself sobbing with feelings I hadn’t touched in three years, a much needed catharsis.
Here it is; the lyrics are below.
When I Leave the World Behind
Irving Berlin, 1915
I know a millionaireI’m so glad to still be alive, alive to keep loving those things for a few more years. Thanks to all of you who were with me then, and thanks to all of you who work today to make a world of better healthcare.
Who's burdened down with care
A load is on his mind
He's thinking of the day
When he must pass away
And leave his wealth behind
I haven't any gold
To leave when I grow old
Somehow it passed me by
I'm very poor but still
I'll leave a precious will
When I must say good-bye
[Refrain:]
I'll leave the sunshine to the flowers
I'll leave the springtime to the trees
And to the old folks, I'll leave the mem'ries
Of a baby upon their knees
I'll leave the night time to the dreamers
I'll leave the songbirds to the blind
I'll leave the moon above
To those in love
When I leave the world behind
[2nd verse:]
To every wrinkled face
I'll leave a fireplace
To paint their fav'rite scene
Within the golden rays
Scenes of their childhood days
When they were sweet sixteen
I'll leave them each a song
To sing the whole day long
As toward the end they plod
To ev'ry broken heart
With sorrow torn apart
I'll leave the love of God
[Refrain:]
I'll leave the sunshine to the flowers
I'll leave the springtime to the trees
And to the old folks, I'll leave the mem'ries
Of a baby upon their knees
I'll leave the night time to the dreamers
I'll leave the songbirds to the blind
I'll leave the moon above
To those in love
When I leave
the world
behind
-
e-Patient Dave
-
1:54 PM
![]() 6 comments
on this post (Click to view or add one)
6 comments
on this post (Click to view or add one)
Sunday, March 28, 2010
TED talk: Intel's Eric Dishman: Take health care off the mainframe
Intel (the computer chip maker) is big into healthcare these days. A lot of people wonder what computer chips have to do with healthcare. At one level you could say that when we all have home health devices, millions more chips will be sold. But as you're about to see, there's a lot more to Intel's thinking than that.
Eric Dishman is director of health innovation and policy for Intel’s Digital Health Group. They're not just talking about what we mean by healthcare today - they're talking about a very, very different approach to what medicine today tries to solve: living better, living longer.
-
e-Patient Dave
-
5:49 PM
![]() 3 comments
on this post (Click to view or add one)
3 comments
on this post (Click to view or add one)
Monday, March 22, 2010
Best License Plate of the Month
Spotted today by daughter Lindsey. Who rocks, btw.
-
e-Patient Dave
-
11:04 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
Saturday, March 20, 2010
Adding the Odiogo blog post reader
I've just added something to this blog that I've seen for years elsewhere: the Odiogo "Voice your content" plugin. Click the "Listen now" button at the top of any post and it'll read it to you.
Pretty amazing, for free. To tell the truth, though I've seen it for years, I've never quite believed it. But it works. :-)
Thanks to two perennial leaders for being the bloggers where I've noticed it:
- Jen McCabe of Health Management RX. (Read her still-extraordinary "I am an e-patient" post from 2008
- Brian Ahier of Healthcare, Technology and Government 2.0. Brian is one of the most down-to-earth, "What makes a difference here?" bloggers in health IT. So it's not surprising that last night when I was looking for a good summary of the current health overhaul bill, I found it on his blog. (It's the second document listed in the post.)
-
e-Patient Dave
-
7:37 AM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Friday, March 12, 2010
Lean retreat, day 5: Reporting to leadership, taking it back to gemba
Here's our class photo. A whole bunch of inspiring residents, some attendings (full doctors, I believe?), some nurses, and a couple of patients:
Of course, this being a major teaching hospital, the leadership provided some, ahem, clear feedback. :-) But this hospital being a great place, the "clear feedback" was delivered respectfully and with good, open dialog.
A big part of our thinking today was about taking it back to gemba - the workplace. Anyone who reads Dilbert knows that too often a retreat like this ends up as an impotent misfire. So our leaders Alice Lee and Julius Yang MD led discussion of how we'll work at bringing these changes to life, while fitting the work into everyone's full workday. I look forward to seeing how it goes.
I pointed out that this process of building bridges, from the "decision room" into the next step, parallels the work we did on the patient discharge process: building a bridge from the staff's intentions out to the patient's home. Without that work, handoffs of either type are unlikely to bear fruit.
__________
I want to say again what a great experience it is to be actively engaged in the process of improving care delivery at my hospital. I know patient engagement isn't new; I'm just so happy to be involved in this way. Believe me, I was a full and active participant, and I wasn't just "surveyed" and sent packing, I was part of the team. What a great experience. And what fun!
-
e-Patient Dave
-
1:56 PM
![]() 1 comment
on this post (Click to view or add one)
1 comment
on this post (Click to view or add one)
Labels: Beth Israel Deaconess, lean, quality improvement
Thursday, March 11, 2010
Lean retreat, day 4: Synchronize / align, and the House of Lean
Yesterday was hard work, because we stepped out of "supposedly" and into "Okay, what CAN we accomplish in 3-6 months?" Because Lean isn't about massive centralized re-engineering, it's about small practical improvements - continuously.
Today we took the results of that work and honed it down to small projects that the hospital will actually pursue. (I didn't realize that when the week started.) The day's byword was "synchronize," not in the time-sync sense, but in the sense of getting aligned and coordinated, rowing in a common direction.
We brought together our different learnings from the week into an action plan that fits into the "house of lean" diagram we started with on Monday. I didn't grab a snapshot of it then, but here's today's hand-drawn reconstruction. See legend below.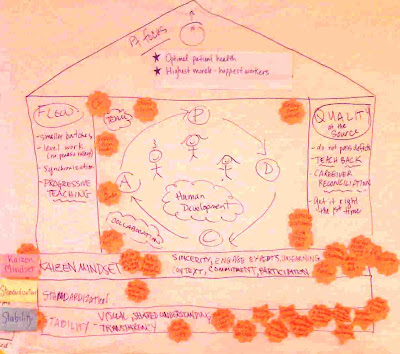
The foundation has three layers:
- Stability: You cannot improve steadily without a stable process. So, a lot of work goes into stabilizing how work is done. In any industry including healthcare this can require giving up a certain amount of craftsmanship - but in my view the predictable, repeatable part of the work is what gets stabilized, and craftsmanship moves out onto the frontiers, where it's most needed.
- Standardization: As I described yesterday, this is about having a shared, continuously improved, agreed approach to the parts of the work that can be standardized.
- "Kaizen mindset": Kaizen is continuous small improvements: every day do something a little bit better.
- Flow: a hallmark of Lean is the idea that inventory and uneven workflow are wasteful. When MIT Sloan's Mike Cusumano went to Japan in the 1980s to study Japan's car makers, he found that although they were all good, Toyota produced the same number of cars with half the floor space and half the people. That's because they managed every aspect of the process to produce steady flow.
Yes, inventory and uneven workload can be managed to a minimal state. And when that happens, all kinds of wasteful workarounds disappear. - Quality at the Source ("Jidoka"): in Lean it's absolute folly to achieve quality by manufacturing defective things and then spending labor to find the defects (inspection) and weed them out. Make everything in a quality fashion the first time.
This week I learned that a vast amount of time on a hospital floor is spent re-checking things because errors are so costly. To me, as someone from industry, this gives the lie to any healthcare executive who takes an arrogant position because of the supposed vast intellect of people in healthcare. I know healthcare executives are smart, but if they're not working on improving quality, they're guilty of ignoring existing knowledge from other disciplines. That's not scientific.
There's another aspect - the center of this house - that doesn't appear in many diagrams of the "House of Lean," but was prominently taught to us today: human development. All lean practitioners talk about "respect for people" or "respect for humanity," but not everyone emphasizes it in this way, as the center of the House. The other day Lean Hospitals author Mark Graban described it to me as respect for human potential, and indeed one of the 8 forms of waste we were taught is "Unused Human Talent."
So you can imagine how pleased I was to be a voice of the patient in this exercise. Because as the week went on, I saw that when we clear out the clutter that keeps clinicians from doing their job, we make it easier for them to make the most of their talent. And by empowering patients and families to be active (participatory medicine), we make the most of their talent too.
What a thrill to be involved in this week. Thanks so much to Beth Israel Deaconess for inviting me and helping to make it possible.
-
e-Patient Dave
-
4:23 PM
![]() 3 comments
on this post (Click to view or add one)
3 comments
on this post (Click to view or add one)
Labels: Beth Israel Deaconess, lean, quality improvement
Wednesday, March 10, 2010
Lean retreat, day 3: The Pig Game (learning about standardized work)
Modern healthcare is complex, and managing complexity is no laughing matter: it can be life and death. (More on this below.) As always this leaves us with the question, what can we do that would make any difference? That's where Lean comes in.
One aspect of Lean is standardized work - where "standardized" means a shared and continuously improved standard approach. Physicians are given leeway to use their judgment, but all in the enterprise must agree that the right way is to agree on a method, all use it, all contribute their ideas for improvement. And track what works.
That's how we know, for instance, that the central line infection rate has dropped so dramatically, as I mentioned the other day.
Well, to teach us about standardized work, today we did a classic Lean exercise: the Pig Game. Everyone is given a "tic tac toe" grid, and instructions on what to draw. In round 1 everyone's pig comes out vastly different, though all had the same spoken instruction. In rounds 2 and 3 .... well, I won't spoil it, but I'll say that the same group of humans produced far more uniform results when the work was defined more effectively. :)
_________
This morning we heard from Steven J. Spear, author of Chasing the Rabbit. For homework we read chapters 2 and 3, which made a compelling case that in today's enterprises complexity is the rule and it's the thing that must be managed: no longer is it sufficient to be good at what each of us does - we must manage, together, the uncontrollably complex interaction between our areas of knowledge.
And yes, when I say "we," I'm including patients. I understand more clearly than ever why patients must be engaged in their care, in and out of the hospital. (Actually that's only true if they want the best possible outcome from their treatment. I do.)
The book relates a heart-rending story of a woman who was accidentally given the wrong fluid and died. I won't try to depict the circumstances because anything short of the whole story would give you the wrong impression; I'll just say that when I read it I cried, not just for the patient but for the nurse who did it. (Apparently the wrong tiny vial, looking almost identical, was in the cart.)
It was heart-rending, as I say; then he documents how very similar failures in process and policy led to NASA's Challenger disaster.
_________
The very first business transformation course I ever took, many years ago, was from a company named Innovation Associates. The course leaders were Charlie Siefert (coincidentally a fellow member of my college glee club) and Peter Senge, who has since become famous for the "Learning Organization" concept, about enterprises whose central competence is to learn new competences. In that course we were taught two fundamentals:
- How to envison a future, unconstrained by current reality. Very right-brain.
- System dynamics: an understanding of how complex systems work. Totally left-brain.
And since in a complex system problems are likely to arise no matter how much you plan, you need to be really honest about how it's going. It's truly inspiring to work with a group that's dedicated to improvement like this. (And producing great results.)
_________
And for the raw-business data junkies out there, here's today's Results Tidbit:
Yesterday I described how the Beth Israel Deaconess business transformation team worked with the orthopedics department. One outcome was a total rework of how hip replacement surgery was done. Not only did they improve quality, they can now schedule three total hip replacements per day, not two.
Yeah, folks, that's a 50% increase in business and better quality.
-
e-Patient Dave
-
8:26 PM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Labels: Beth Israel Deaconess, lean, quality improvement
Tuesday, March 9, 2010
Lean retreat, day 2
Previous post here
Continuing our exploration of how to reduce how many Medicare patients are readmitted after leaving the hospital, this morning we started getting our hands dirty, thinking out all the activities that take place - and can go wrong - when a patient is sent home.
Now, I have some experience with this, having been sent home seven times from my seven admissions in 2007, but I never had any idea how many things were going on behind the scenes. In particular I had no clue how often "final" paperwork (in the computer) had to get "unfinalized" and modified - and much how of a pain the computer systems make it. Plus, there are many many places where information can fall through the cracks, because this is all far less automated than I would have, naively, thought.
As always, the useful question quickly becomes, what can we do to improve this? It's no good ranting, because even a rant leaves you with this: "Okay, got it. Now: you're at where you're at. What can we do that will make any difference?" And here's where it gets inspiring, because Lean has produced remarkable results without requiring vast new IT systems, and especially since its methods are well within the reach of ordinary people. For one thing, you don't have to figure it all out first - you think, and try things, and see what works. For another, today's eye-opening exercise was done with Post-Its, paper, and Sharpies.
And here's where it gets inspiring, because Lean has produced remarkable results without requiring vast new IT systems, and especially since its methods are well within the reach of ordinary people. For one thing, you don't have to figure it all out first - you think, and try things, and see what works. For another, today's eye-opening exercise was done with Post-Its, paper, and Sharpies.
More formally, "think, try, see what works" is called PDCA: Plan, Do, Check, Act [or Adjust]. It's really the scientific method applied to practical managerial problem solving. And it works. I've personally witnessed the transformation of the customer experience in this hospital's orthopedics department; when I first went there the wait was horrid (three hour visits were not unusual), and today people are in and out in 52-56 minutes - consistently.
This stuff works.
In the exercise pictured here, we mapped out four different stages of a patient being discharged, going home, and eventually returning to the clinic (doctor's office) for a follow-up visit. Apologies for the poor picture, but you can vaguely see "swim lanes" for the different people involved: the top row, with green Post-Its, is the patient; the row below is the case manager; other rows are the inpatient MD, the nurse, pharmacist, etc. All these people have specific responsibilities in discharging a patient. Each activity was written on a stickie. There were hundreds.
Then we went back and, as a group, looked at every single activity and marked it in the Lean way:
- Value Added. (Is this specific activity something the customer came here for?) Getting instructions or therapy: yes. Waiting: no.
- Not Value Added. Everything else: filling out paperwork, re-checking medication lists, paging the attending physician, you name it. Some might be necessary, but none of them is what the customer came here for. Lean strives to eliminate these.
- Not Value Added, but Required. A subset of Not Value Added.
Yellow and orange stickies, known as "stormclouds," were added, showing areas where things can go awry. Clusters indicate key areas to engineering reliability into the process.
Does it work? Heck yes: more data on that in tomorrow's installment.
-
e-Patient Dave
-
7:26 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
Labels: Beth Israel Deaconess, lean, quality improvement
Monday, March 8, 2010
Participating in my hospital's Lean quality improvement retreat
I'm very, very honored to be indulging this week in a new form of "patient engagement": I'm participating in the annual "Lean" quality improvement retreat at my hospital, Boston's Beth Israel Deaconess Medical Center.
In the workshop with me are about 20 BID staffers - mostly residents, some nurses and other staff. Having been on the receiving end of care in seven admissions during my near-fatal 2007 illness, it's an honor to be behind the scenes now and helping work on the continuous improvement that's a hallmark of Lean. Here's the team leading the workshop, from the hospital's Business Transformation team. From left: Jenine Davignon, Kim Eng, Julius Yang, Bonnie Baker, Alice Lee, Anjala Tess.
Here's the team leading the workshop, from the hospital's Business Transformation team. From left: Jenine Davignon, Kim Eng, Julius Yang, Bonnie Baker, Alice Lee, Anjala Tess.
"Lean" is the methodology that's transformed many industries in recent decades. It's about identifying what you do that creates value for your customer - as defined by the customer - and eliminating everything you do that's not that. Marvelously, when you follow this method, not only does quality go up but costs go down, and things tend to get done faster, too - a pretty slick combination.
Hospital CEO Paul Levy has written often on his blog about how they've been applying Lean methods for five years. A recent example is here. In this workshop we're all learning about the Lean approach, and even on our first day we applied it by "going to gemba," the place where work happens.
Our homework is from the book Lean Hospitals by Mark Graban of the Lean Enterprise Institute in Cambridge. He was the guest lecturer during today's working lunch.
The focus of our workshop this week is the hospital discharge process. I never would have known it's such a big deal, but it turns out nationwide 20% of all patients discharged from hospitals are readmitted within a month - and Beth Israel Deaconess is a bit worse than that. So we'll be looking at all the various factors that might contribute to unsuccessful handoffs, and how process improvements might help.
This place has some success with Lean. One of the first big initiatives was to reduce the rate of central line infections. In January Paul announced that the infection rate per 1,000 patient days has dropped 83%. To me this is a big deal because:
- 25% of central line infections lead to death
- During my treatment in 2007, I had four central lines put in, for a total of 28 days.

So before my admission I'd read all about this initiative, and I was able to chat about it with the surgeons each time they did it to me. And I was, like, really glad they'd undertaken this Lean improvement before my time came.
That kind of openness is only possible if you're committed to improvement, more than anything else.
That's part of why I'm honored and thrilled to be part of their next Lean workshop. So much in healthcare needs improving, and here we are, actively at work on making caregivers' jobs more effective.
Next post in the series here
-
e-Patient Dave
-
9:20 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
Labels: Beth Israel Deaconess, lean, quality improvement
Saturday, March 6, 2010
Impromptu interview with the Get Better Health team
This past week I attended the big annual convention of HIMSS, the Health Information Management Systems Society, in Atlanta. While there I was buttonholed by the famous Dr. Val Jones of Get Better Health to come talk on their live video stream. It's a fun thing - all you need is a webcam, and you can broadcast like this!
We talked a little about the show and then got into some (unexpectedly) sincere talk about what e-patient is and isn't, what participatory medicine is about, etc.
My host here was the anonymous doctor blogger Doctor Anonymous.
-
e-Patient Dave
-
4:18 PM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Friday, March 5, 2010
News for cancer patients: Attitude influences outcomes
I've often described how when the odds were really poor, I used the power of the mind to help my own cause.I cited Norman Cousins' famous book Anatomy of an Illness, I asked my family to send me DVDs of things that make me laugh, and throughout my disease, when I or others were faced with worries, I asked "What could be said that would make a difference?"
I've cited that when Cousins wrote his book we didn't yet know about psychoneuroimmunology - the relatively new field of how mood affects the nervous system which affects the immune system. In other words, yeah, your mood can make you strong. (I'm not kidding; look it up.)
On Twitter today I came across a blog post about some evidence that people with optimistic personalities do better years later when lung cancer strikes.
- 534 lung cancer patients were selected who had, years earlier, taken the MMPI personality test.
- They were divided into "pessimistic" and "non-pessimistic." The "non" group might include optimistics and neutrals - I don't know.
- Their survival rates were monitored.
- 46% higher median survival than pessimists
- 55% higher 5 year survival
So: Regardless of whether your medical condition is strong or not, this sounds like a heck of a good thing to add to your tactics. Doesn't cost much, either.
Presuming you want to live longer, that is. You don't have to. But if you do, think about it.
The original article appeared in the Journal of Thoracic Oncology. The summary that I read is on Medical News Today.
-
e-Patient Dave
-
11:12 PM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Labels: advice for cancer patients
Tuesday, February 16, 2010
Interview with Pixels & Pills at the ePharma Summit
Last week I was honored to be part of a presentation at the ePharma Summit in Philadelphia. I was sponsored by Klick!, a Toronto company I visited in December after meeting them at the ePatient Connections conference in October. I've seen a lot of Web 2.0 and Health 2.0 things over the years, and I was blown away by the instructional quality and the user experience of the websites Klick creates to engage consumers. And for their healthcare business, that means patients. Real "help you help yourself" sites.
At the session in Philadelphia, I spoke with Klick's Brian O'Donnell. His topic was "Value-Add Beyond the Pill," talking to pharma marketers about why and how they should engage with patient communities - adding value beyond just the medication they sell. During Brian's talk, I presented my first-hand experience as an engaged patient using the internet during my illness. (I hope video of that talk will be available.)
Afterward, I took my turn in the side room where Pixels&Pills (an online marketing agency) was doing live interviews. I was hoarse (still getting over a cold) but that never stopped me from talking.:)
- What's all this about "patient is not a third person word"?
- Say something about the new Society for Participatory Medicine and its Journal of Participatory Medicine.
- What is the role of the physician in a world where patients are more involved in their care?
- How can communication between patients and physicians be better fostered?
- Are more and more patients really going online for medical information?
Thanks to Pixesl&Pills and again to Klick for this opportunity.
-
e-Patient Dave
-
5:37 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)
A dose of laughter medication
I've written before about the medical and emotional value of laughing one's butt off. (Example from December here.) I hereby strongly endorse this particular formulation.
(Email subscribers: if you can't see the video, click here.)
-
e-Patient Dave
-
3:58 PM
![]() 0 comments
on this post (Click to view or add one)
0 comments
on this post (Click to view or add one)
Labels: humor
Thursday, January 28, 2010
3 years ago I was out of time. Now I'm in it.
Yesterday's edition of this had a wrong link. Apologies.
Three years ago this week I got my formal diagnosis. This week:
Last Sunday the New Hampshire Union Leader ran a story "What's next for health care" following the Massachusetts Senate election. For some reason, I'm happy to say, they led with my sentiment that I just want people to be able to get good care when they need it.
At the end of the interview I learned that the reporter's mother had died of cancer 5 years ago.
Then this piece appeared online today, for tomorrow's print edition of Time. Again somehow they put my story first.
Honestly I think what's doing this is that I always hammer on the point "This is personal. Your time will come." Don't I know it.
And, as fate would have it, this is happening unexpectedly in a week when I'm in DC, speaking at some conferences and meeting executives of non-profits. Yesterday I decided to visit my legislators' staff on Capitol Hill; I met with one yesterday and have appointments with the others tomorrow. AWFULLY convenient that I can have this publicity in hand when I walk in!
The universe works in mysterious ways. This time, I'll take it.
-
e-Patient Dave
-
11:32 PM
![]() 3 comments
on this post (Click to view or add one)
3 comments
on this post (Click to view or add one)
Sunday, January 10, 2010
#GetUpAndMove, music, and "the fun theory"
Twitter friend and outrageous visionary Jen McCabe is a brilliant thinker with a San Francisco startup company called "Get Up And Move." It's a free social media way of encouraging people to, well, get up and move. (Don't I love things that are exactly what they say?)
Its URL is the fun GetUpAndMove.Me, and its tagline is "Barter with Exercise." Go look at it. At present it's only tied in to Twitter (hashtag #getupandmove), but they're working on Facebook.
I've never been an exercise fiend, but GetUpAndMove has led to my discovering that I like doing a couple of minutes of exercise if I do it to a song. The radio site blip.fm has a ton of great songs (to play for free), so for instance if I agree to do a minute of pushups, I start one of my songs and do it. Examples:
- Soul Sacrifice (Santana at Woodstock)
- Little Deuce Coupe (Beach Boys)
- Ecstatic R&B love song introduced to me long ago by friend Frank Moore: Don't Leave Me This Way - starts modest and builds. Great for jumping jacks
- And my personal anthem: Play That Funky Music, White Boy
Today in the email from a chorus buddy I got this video, and realized this is what makes "GUAM" (as its fans call it) work for me, when so much hasn't: fun.
(I add music, but with or without it, there's the fun of challenging people, and publicly trash-talking your challenger or challengee.)
Here's to Jen, here's to Frank, here's to innovation, and here's to fun. Get up and move!
-
e-Patient Dave
-
1:05 PM
![]() 2 comments
on this post (Click to view or add one)
2 comments
on this post (Click to view or add one)




